Pulmonary Tuberculosis: What You Need to Know
Pulmonary tuberculosis (TB) is a lung infection caused by the bacteria Mycobacterium tuberculosis. It spreads when an infected person coughs, sneezes, or talks, releasing tiny droplets that others can inhale. Most people think of TB as a disease from the past, but it still affects millions worldwide and can hit anyone.
If you’ve ever wondered whether a lingering cough means TB, the answer lies in the details. A cough lasting more than three weeks, night sweats, unexplained weight loss, and fever are classic red flags. Some folks also notice chest pain or coughing up blood-tinged sputum. These signs don’t guarantee TB, but they’re enough to prompt a medical check‑up.
How to Spot the Signs
The first step is recognizing symptoms early. A persistent cough that doesn’t improve with over‑the‑counter remedies should raise concern. Pair that with fatigue that won’t go away, and you have a reason to see a doctor. TB often mimics other respiratory illnesses, so doctors use specific tests to confirm it.
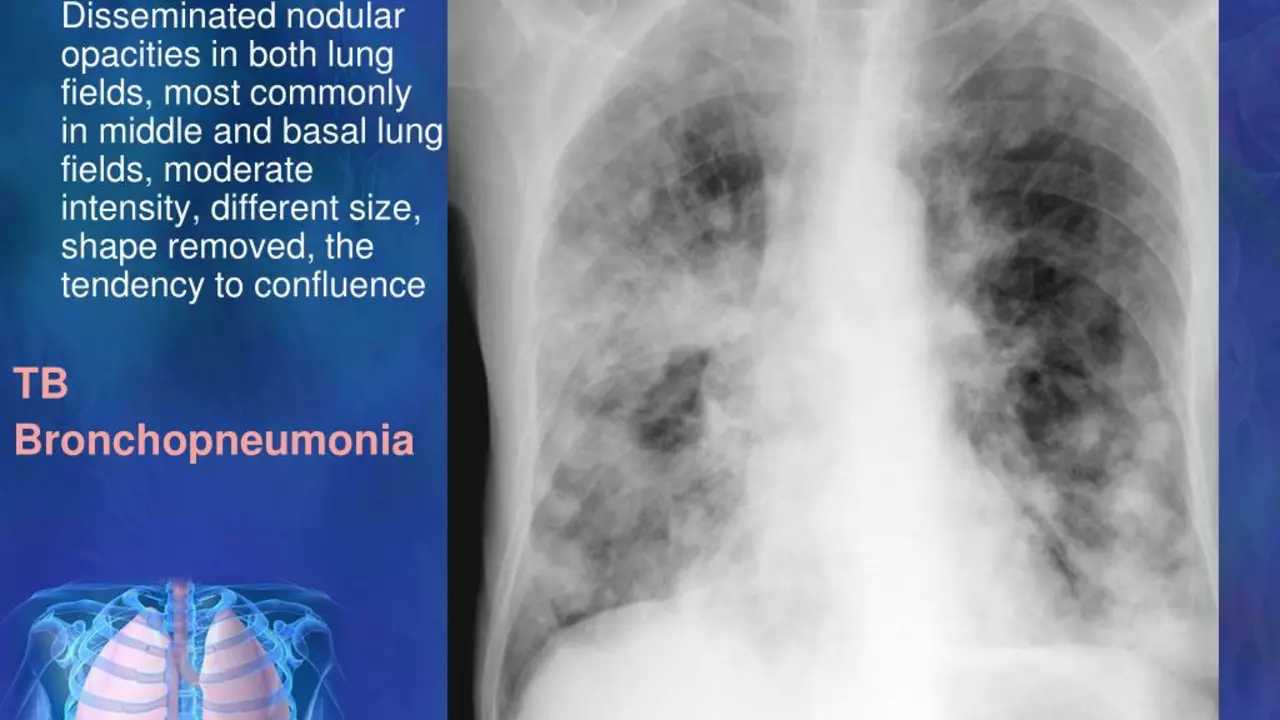
Diagnostic tools include a chest X‑ray, sputum smear microscopy, and molecular tests like GeneXpert. The sputum test looks for the bacteria directly, while the X‑ray shows lung damage patterns typical of TB. Modern labs can even detect drug‑resistant strains in a single visit, helping doctors choose the right medication early.
Treating & Preventing TB
Treatment is straightforward but requires commitment. The standard regimen, known as “DOT” (directly observed therapy), combines four antibiotics—isoniazid, rifampicin, ethambutol, and pyrazinamide—for the first two months, followed by a continuation phase of isoniazid and rifampicin for four more months. Sticking to the schedule prevents relapse and stops drug‑resistant TB from emerging.
Side effects like nausea, liver strain, or skin rash can happen, so regular check‑ups are essential. If you experience severe reactions, your doctor may adjust doses or switch drugs.
Prevention focuses on vaccination and infection control. The BCG vaccine offers partial protection, especially in children, by training the immune system to fight TB bacteria. In high‑risk settings—like shelters, prisons, or clinics—proper ventilation, mask use, and prompt isolation of suspected cases curb spread.
For anyone worried about exposure, a simple test called a tuberculin skin test (TST) or an interferon‑gamma release assay (IGRA) can tell if you’ve been infected. If the result is positive but you feel fine, doctors may prescribe preventive therapy to stop active disease from developing.
Living with TB doesn’t mean you have to isolate forever. After a few weeks of treatment and once you’re no longer contagious, normal life resumes. Maintaining good nutrition, avoiding smoking, and staying on medication are the best ways to recover fully.
If you suspect TB, don’t wait. Early diagnosis saves lives, reduces transmission, and makes treatment easier. Use these pointers as a quick checklist: persistent cough, night sweats, weight loss, fever, and any blood in sputum—then seek professional care.
The Role of Vaccination in Preventing Pulmonary Tuberculosis
- Jul, 1 2023
- 13
In my latest research, I delved into the significant role of vaccination in preventing pulmonary tuberculosis. I found that the BCG vaccine, particularly administered at birth, plays a crucial part in providing protection against severe forms of Tuberculosis in children. Interestingly, its effectiveness in adults is a bit variable, yet it's still a key player in TB prevention. I also learned about the ongoing development of new vaccines, which aims to provide a more consistent and effective response against all forms of TB. This highlights the importance of global efforts in enhancing TB vaccination strategies to combat this deadly disease.
Categories
- Health and Medicine (76)
- Health and Wellness (57)
- Medicine (37)
- Women's Health (11)
- Mental Health (10)
- Men's Health (7)
- Beauty and Wellness (4)
- Health Information (4)
Archives
- April 2026 (1)
- March 2026 (11)
- February 2026 (11)
- January 2026 (25)
- December 2025 (28)
- November 2025 (25)
- October 2025 (27)
- September 2025 (14)
- August 2025 (3)
- July 2025 (2)
- June 2025 (2)
- May 2025 (3)
- online pharmacy
- medication safety
- generic drugs
- dietary supplement
- health benefits
- dietary supplements
- prevention
- fertility
- online pharmacy Australia
- side effects
- QT prolongation
- medication side effects
- diabetes medications
- GLP-1 agonists
- nocebo effect
- brand vs generic
- treatment
- treatment options
- benefits
- connection
