PCOS – What You Need to Know
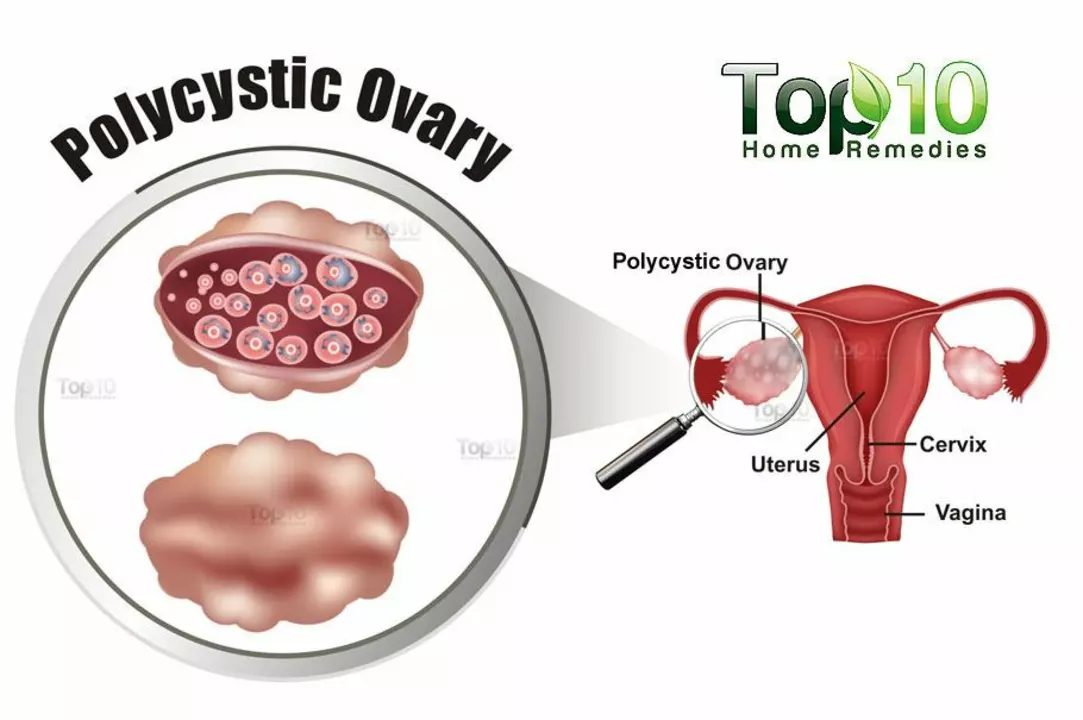
If you’ve heard the term PCOS but aren’t sure what it really means, you’re not alone. Polycystic ovary syndrome (PCOS) is a hormonal condition that affects many women of reproductive age. It’s not just about “cysts” on the ovaries – those tiny follicles are often a side effect, not the main problem.
In PCOS, your ovaries produce more androgens (male‑type hormones) than usual. This hormonal imbalance can throw off your menstrual cycle, make it harder to get pregnant, and cause a range of other symptoms. The good news is that there are clear steps you can take to feel better, from simple diet tweaks to proven medications.
Common Symptoms & Diagnosis
The first sign most women notice is an irregular period – maybe you’re skipping months or bleeding heavily when it does come. Other red flags include unwanted facial or body hair, acne that won’t clear up, and stubborn weight gain around the belly.
Doctors usually confirm PCOS with a combo of blood tests (to check hormone levels) and an ultrasound to look at the ovaries. You don’t need every test to get started; if you have two out of three classic signs – irregular periods, excess hair growth, and polycystic‑looking ovaries – a diagnosis is often made.
Managing PCOS: Lifestyle and Medications
The cornerstone of PCOS care is lifestyle. Cutting back on refined carbs and sugary drinks can lower insulin spikes, which in turn helps balance hormones. Aim for whole grains, lean proteins, plenty of veggies, and a steady intake of healthy fats like avocado or nuts.
Exercise isn’t just about weight loss; regular cardio and strength training improve insulin sensitivity and can smooth out menstrual cycles. Even 30 minutes a day, five days a week, makes a difference.
If diet and exercise aren’t enough, doctors often prescribe medications. Birth control pills are a common first‑line choice because they regulate periods and reduce androgen levels. Metformin, a diabetes drug, is another option that helps the body use insulin more effectively and can aid weight management.
For women trying to conceive, fertility drugs such as clomiphene or letrozole may be recommended. These stimulate ovulation without fixing the underlying hormone imbalance, but they’re effective for many who want to get pregnant.
Supplements can also play a supportive role. Inositol (especially myo‑inositol) has shown promise in improving insulin resistance and restoring regular cycles. Vitamin D deficiency is common in PCOS, so checking your levels and supplementing if needed can boost overall health.
Remember, every woman’s experience with PCOS is unique. What works for one person might need tweaking for another. Keep a symptom diary, stay in touch with your healthcare provider, and don’t be afraid to ask questions about any new treatment.
Bottom line: PCOS can feel overwhelming, but with the right mix of diet, exercise, and medical support you can take control of your symptoms and improve quality of life. Start small, stay consistent, and watch the changes add up over time.
The Relationship Between Fertility and Polycystic Ovary Syndrome (PCOS)
- Jun, 2 2023
- 16
As someone who has been researching PCOS, I've discovered that this hormonal disorder can have a significant impact on a woman's fertility. It's estimated that nearly one in ten women of childbearing age are affected by PCOS, making it a common cause of infertility. The hormonal imbalances associated with PCOS often lead to infrequent or absent ovulation, making it difficult for women to conceive. Furthermore, PCOS can also increase the risk of miscarriage and other pregnancy complications. It's crucial for women with PCOS to work closely with their healthcare providers to manage their symptoms and increase their chances of a successful pregnancy.
Categories
- Health and Medicine (77)
- Health and Wellness (57)
- Medicine (37)
- Women's Health (11)
- Mental Health (10)
- Men's Health (7)
- Beauty and Wellness (4)
- Health Information (4)
Archives
- April 2026 (2)
- March 2026 (11)
- February 2026 (11)
- January 2026 (25)
- December 2025 (28)
- November 2025 (25)
- October 2025 (27)
- September 2025 (14)
- August 2025 (3)
- July 2025 (2)
- June 2025 (2)
- May 2025 (3)
- online pharmacy
- medication safety
- generic drugs
- dietary supplement
- health benefits
- dietary supplements
- prevention
- fertility
- online pharmacy Australia
- side effects
- QT prolongation
- medication side effects
- diabetes medications
- GLP-1 agonists
- nocebo effect
- brand vs generic
- treatment
- treatment options
- benefits
- connection
