Liver Function Tests Explained: ALT, AST, Bilirubin, and What They Really Mean
 Mar, 6 2026
Mar, 6 2026
When your doctor orders a liver function test, it’s not because you have a hangover. It’s because something in your blood is telling them your liver might be under stress. But here’s the thing: liver function tests don’t actually measure how well your liver works. They measure damage. And that’s a big difference.
Think of it like checking your car’s check engine light. The light doesn’t tell you if the engine is running efficiently-it just says something’s wrong. That’s what ALT, AST, and bilirubin do. They’re warning signs. And if you don’t know how to read them, you might panic over a small flicker-or miss a siren.
What You’re Really Measuring
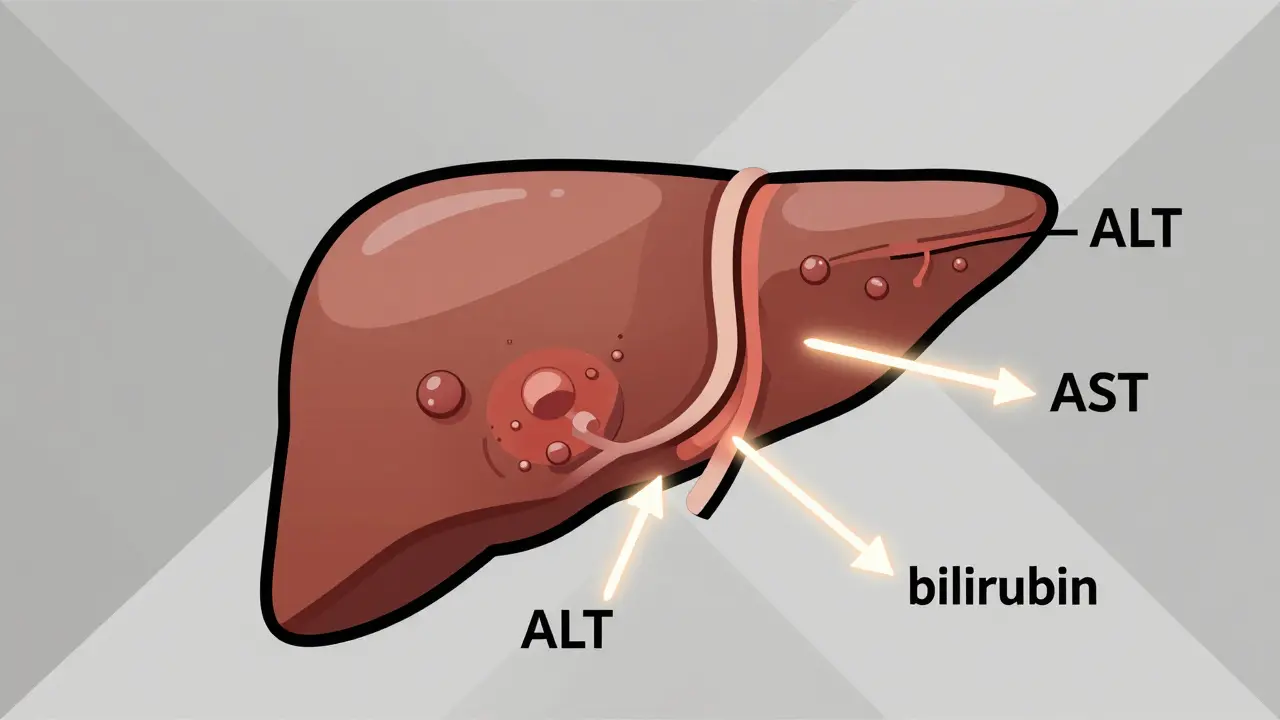
Most people think of liver function tests as one thing. But they’re really three different stories rolled into one blood panel. The three most common markers-ALT, AST, and bilirubin-each tell a different part of the story.
ALT (alanine aminotransferase) is mostly found in liver cells. When those cells get damaged, ALT leaks into the blood. It’s the most specific marker for liver injury. If your ALT is high, it’s almost always pointing to your liver.
AST (aspartate aminotransferase) is trickier. Yes, it’s in the liver, but it’s also in your heart, muscles, and even your kidneys. A high AST could mean liver damage… or a rough workout, a heart attack, or even muscle breakdown. That’s why you never look at AST alone.
Bilirubin is a yellow pigment made when your body breaks down old red blood cells. Your liver processes it and sends it out in bile. If bilirubin builds up in your blood, your skin or eyes turn yellow-that’s jaundice. But even before you look yellow, your blood test will show it’s rising.
Reference ranges vary by lab, but generally:
- ALT: 7-55 U/L
- AST: 8-48 U/L
- Total bilirubin: 3-17 μmol/L
And here’s the catch: normal doesn’t always mean healthy. Men tend to have higher normal levels than women. People with higher BMI often have ALT and AST levels 10-15% higher-even if their liver is fine. So if you’re a 90kg man with a BMI of 29, your “normal” might be 60 U/L for ALT. That doesn’t mean you’re sick. It just means your lab’s reference range isn’t one-size-fits-all.
Patterns Matter More Than Numbers
One number on its own doesn’t tell you much. It’s the pattern that cracks the case.
Let’s say your ALT is 120 U/L and AST is 80 U/L. That’s elevated, sure. But what does it mean? Here’s how to break it down:
- If ALT is higher than AST (ALT > AST), you’re likely looking at non-alcoholic fatty liver disease (NAFLD), now called MASLD (Metabolic dysfunction-Associated Steatotic Liver Disease). This is common in people with obesity, diabetes, or high cholesterol.
- If AST is higher than ALT-especially if AST is more than twice ALT-you’re probably looking at alcohol-related liver damage. In alcoholic hepatitis, the AST:ALT ratio is often 2:1 or higher.
- If both ALT and AST are above 500 U/L, it’s usually acute liver injury. Think viral hepatitis (like hepatitis A or B), a drug reaction (especially paracetamol overdose), or a sudden lack of blood flow to the liver (ischemic hepatitis).
- If ALT and AST are only slightly up-say, 40-80 U/L-it could be nothing. Studies show 10-15% of healthy people have mild elevations with no liver disease. A 2022 JAMA Internal Medicine study found that nearly 4 out of 10 primary care doctors ordered unnecessary scans for these mild rises.
Now, what if your ALT is normal, but bilirubin and ALP (alkaline phosphatase) are high? That’s a different story. This pattern screams cholestasis-a blockage in bile flow. It could be gallstones, a tumor, or a medication like antibiotics or birth control pills. When ALP is high and GGT (gamma-glutamyl transferase) is also up, it confirms the problem is liver-related. But if ALP is high and GGT is normal? Look at your bones. ALP comes from bone tissue too. A fracture or bone disease can mimic liver trouble.
Why Bilirubin Tells You About Blockages
Bilirubin has two forms: unconjugated (old, unprocessed) and conjugated (processed by the liver). Total bilirubin adds them up. But if you look at direct (conjugated) bilirubin, you can see if the liver is struggling to push bile out.
If direct bilirubin is high, your liver is making the bilirubin fine, but it can’t get it out. That’s a blockage. Think bile duct stones, strictures, or even pancreatic cancer pressing on the duct. If unconjugated bilirubin is high, it’s more about your body breaking down too many red blood cells (hemolysis) or your liver not being able to process the load (like in Gilbert’s syndrome-a harmless, common condition).
And here’s a fact most people miss: bilirubin doesn’t spike overnight. It builds slowly. So if your bilirubin jumps from 10 to 50 μmol/L in a week, that’s urgent. If it’s been 15 for six months? Probably not a crisis.

Albumin and Prothrombin Time: The Real Function Test
Here’s where people get fooled. ALT and AST are damage sensors. But albumin and prothrombin time (PT) are the only tests that actually measure what your liver does.
Albumin is a protein your liver makes. It keeps fluid in your blood vessels, carries hormones, and helps with healing. If your albumin is low-below 35 g/L-it means your liver has been struggling for months. It takes 20 days for your body to make new albumin. So a low level isn’t about a recent hangover. It’s about chronic damage: cirrhosis, long-term alcohol use, or severe malnutrition.
Prothrombin time measures how fast your blood clots. Your liver makes clotting factors. If your PT is prolonged (INR is high), your liver can’t make enough of them. This is a red flag for acute liver failure. It can happen fast-within days-after a drug overdose or severe viral hepatitis.
These two markers are the difference between “your liver got bruised” and “your liver is failing.” One tells you about injury. The other tells you about survival.
When to Worry-and When to Chill
Not every elevated number needs a biopsy. In fact, most don’t.
Here’s what the guidelines say:
- If ALT or AST are under 2x the upper limit (so under 110 U/L for ALT), and you have no symptoms, no jaundice, no alcohol use, and no risk factors-monitor it. Repeat the test in 3-6 months. Many times, it goes back to normal.
- If ALT or AST are above 500 U/L, or they’re rising fast (more than 100 U/L per week)-get seen now. This could be drug-induced, viral, or ischemic injury.
- If you have jaundice, dark urine, pale stools, or abdominal swelling-don’t wait. Go to urgent care.
- If you drink alcohol regularly and your AST is twice your ALT? That’s a strong signal. Cut back. Get a liver ultrasound.
And here’s something you won’t hear from your GP often: NAFLD/MASLD is silent until it’s advanced. Most people with fatty liver have no symptoms. No pain. No fatigue. Just a slightly high ALT. But over time, it can turn into inflammation (steatohepatitis), then scarring (fibrosis), then cirrhosis. That’s why a simple blood test today could prevent a transplant in 10 years.
The Bigger Picture: LFTs Are Just One Piece
A 2021 study of over 12,000 patients showed that using LFTs alone to predict advanced liver scarring was only 68% accurate. But when doctors combined them with a simple score called FIB-4 (which uses age, platelets, ALT, and AST), accuracy jumped to 89%.
That’s the future of liver care. Blood tests + simple calculations + ultrasound = early detection. No biopsy needed.
And it’s not just about alcohol or drugs. The rise of obesity, diabetes, and metabolic syndrome means more people than ever have fatty liver. In fact, MASLD is now the most common liver disease in the world. And it’s often found by accident-on a routine blood test.
So if your ALT is 55, and you’re 45, and you eat takeout three times a week? Don’t panic. But do something. Cut sugar. Walk 30 minutes a day. Lose 5% of your body weight. You might reverse it.
The liver is one of the few organs that can regenerate. But only if you give it a chance.
Can mild elevations in ALT and AST mean nothing?
Yes. Up to 15% of healthy people have ALT or AST levels slightly above the normal range without any liver disease. Factors like obesity, intense exercise, or even recent illness can cause small rises. If levels are under 2x the upper limit and stable over time, monitoring is usually enough-no need for scans or biopsies.
Why is AST higher than ALT in alcohol-related liver disease?
Alcohol damages liver cells in a way that releases more AST than ALT. Also, alcohol can affect muscle tissue, and AST is found in muscle. The AST:ALT ratio is usually above 2:1 in heavy drinkers. If the ratio is over 2, alcohol is likely the cause-unless there’s another explanation like heart damage or muscle injury.
Can bilirubin be high without liver disease?
Yes. Gilbert’s syndrome is a harmless genetic condition where the liver doesn’t process bilirubin efficiently. It causes mild, intermittent jaundice, especially during stress or fasting. It doesn’t cause liver damage and needs no treatment. If GGT and ALP are normal, and only unconjugated bilirubin is high, Gilbert’s is likely.
Does a normal LFT mean my liver is healthy?
Not necessarily. Early fatty liver (MASLD) often shows normal ALT and AST. The liver can be damaged without leaking enzymes. That’s why doctors now use ultrasound or FibroScan to detect fat and scarring even when blood tests look fine. LFTs are a screen, not a full check.
How long does it take for ALT to return to normal after liver injury?
ALT has a half-life of about 47 hours, meaning it takes roughly 3-7 days to drop by half after the injury stops. Full recovery can take weeks, depending on the cause. In acute viral hepatitis, ALT may stay elevated for months. If it doesn’t improve after 3 months, further investigation is needed.
What to Do Next
If your LFTs are abnormal, don’t rush to Google. Don’t panic. Don’t quit alcohol overnight and expect instant results. Do this:
- Check your numbers against your lab’s reference range-not someone else’s.
- Look at the pattern: Is it ALT-dominant? AST-dominant? Is bilirubin up? Is albumin low?
- Ask: Do I have symptoms? Do I drink? Am I overweight? Do I take supplements or painkillers?
- Repeat the test in 6-12 weeks. If it’s still up, ask for an ultrasound or FIB-4 score.
- Focus on lifestyle: cut sugar, lose weight, move more. That’s the most effective treatment for fatty liver.
Your liver doesn’t need a miracle. It needs space. Space from toxins. Space from excess fat. Space from neglect. Give it that, and it will heal itself-more often than you think.

phyllis bourassa
March 7, 2026 AT 16:02Susan Purney Mark
March 9, 2026 AT 01:51Ian Kiplagat
March 10, 2026 AT 16:04amber carrillo
March 10, 2026 AT 22:47Tim Hnatko
March 11, 2026 AT 22:10Aaron Pace
March 13, 2026 AT 11:55Joey Pearson
March 15, 2026 AT 04:36Roland Silber
March 16, 2026 AT 04:00Patrick Jackson
March 16, 2026 AT 08:32